Pulmonary Tuberculosis (PTB), an infection of the lungs that occurs upon inhalation of Mycobacterium tuberculosis (MTB), affects nearly 10 million people per year worldwide.
A retrospective study conducted at Pusan National University School of Medicine in South Korea revealed that healthcare workers performing bronchoscopies are subjected to an increased incidence of MTB exposure as a result of unexpected PTB, when patients have not been diagnosed with MTB infection.
Symptoms of MTB infection include coughing, chest pain, and bloody sputum, of which coughing greatly exacerbates the highly infectious nature of the disease. Those who come into close contact with PTB patients are at risk for MTB infection.
In some cases, the infection can be latent, as in a lack of visible symptoms from patient who is highly infectious. Unexpected PTB occurs as a result of misdiagnosis or an absence of diagnosis, and can put healthcare workers at increased risk for MTB exposure.
Of particular risk are workers who perform bronchoscopies, in which bronchioscopic specimens and post-bronchoscopy sputum are collected to diagnose various lung diseases.
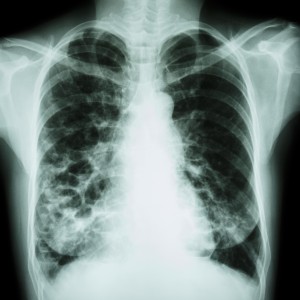 Bronchoscopy is a crucial method for diagnosing a range of lung diseases, including lung cancer, cystic fibrosis, chronic obstructive pulmonary disease (COPD), and PTB.
Bronchoscopy is a crucial method for diagnosing a range of lung diseases, including lung cancer, cystic fibrosis, chronic obstructive pulmonary disease (COPD), and PTB.
In the case of PTB diagnosis, current guidelines recommend that the healthcare workers utilize higher-grade respiratory precaution to prevent exposure to MTB. But no current guidelines exist to protect healthcare workers from exposure to unexpected PTB.
While the US maintains a low prevalence of PTB, countries such as India and South Korea have high and intermediate prevalence of PTB, respectively. The incidence of unexpected occupational MTB exposure by healthcare workers performing bronchoscopies could be higher in these countries, warranting stricter guidelines.
Using data from Pusan National University Hospital during 2011-2013, the authors examined 1,650 cases of bronchoscopies performed on patients who were diagnosed with ‘a respiratory disease other than PTB.’ Of the patient cohort, 76 were ultimately diagnosed with PTB post-bronchoscopy, making 4.6% of the cases of ‘respiratory disease other than PTB’ actually unexpected PTB. This percentage suggests an increased incidence of exposure to MTB by healthcare workers performing bronchoscopies.
The results emphasize the need for more stringent guidelines regarding the utilization of higher-grade respiratory precaution during bronchospies – regardless of whether the presumptive diagnosis suggests an MTB infection – in countries that have intermediate or high prevalence of PTB.
The retrospective study also identified independent risk factors associated with unexpected PTB diagnosis, including the presence of anthracofibrosis, bronchiectasis, and atelectasis on CT scans prior to bronchoscopy. This finding adds more specificity to circumstances and patient symptoms which also warrant increased stringency during the procedure.
In summary, healthcare workers performing bronchoscopies are subject to a higher incidence of unexpected occupational exposure to MTB. This is a preventable outcome which can be mitigated by employing strict guidelines for the use of higher-grade respiratory barriers during the procedure, even without PTB diagnosis of the patient.

