No U.S. Food and Drug Administration (FDA)-approved antibiotics exist for people with bronchiectasis, making the condition extremely challenging to treat and manage. However, several antibiotics are used “off-label” — meaning that the FDA approved the medications for other diseases. Scientists are also in the process of developing new treatments for bronchiectasis, or are testing treatments developed for other conditions, specifically in bronchiectasis, for the first time.
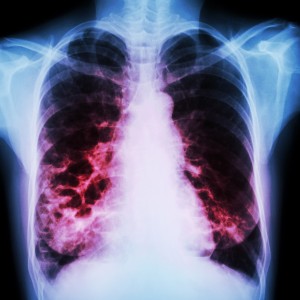 Bronchiectasis causes damage to the tubes that carry air in and out of the lungs. Airways become scarred and weak, and are therefore less effective at delivering oxygen to the body.
Bronchiectasis causes damage to the tubes that carry air in and out of the lungs. Airways become scarred and weak, and are therefore less effective at delivering oxygen to the body.
According to the American Lung Association, “Bronchiectasis can occur as part of a birth defect or as a result of injury or other diseases, like tuberculosis, pneumonia and influenza. It also can be caused by a blockage in your airways due to a growth or something you inhaled as a child such as a piece of a toy or peanut.”
Bronchiectasis usually occurs when there is an infection preventing mucus clearing. Mucus is important to remove inhaled dust, bacteria, and other tiny particles. When mucus lingers it encourages the growth of bacteria and further infection, creating a vicious cycle of increased infection and damage. Ultimately, respiratory failure and heart failure can result.
A recent article, aptly titled “Bronchiectasis: which antibiotics to use and when?” appeared in the March 11 issue of Current Opinion in Pulmonary Medicine. The paper summarizes the current understanding of and options for antibiotic treatment in bronchiectasis.
According to the report, “Since 2012, a number of manuscripts have been published that provide evidence to support the use of antibiotics in non-[cystic fibrosis] bronchiectasis, including macrolide antibiotics, inhaled amino glycosides and inhaled fluoroquinolone therapies. However, data remain preliminary and there are phase 3 trials underway to further investigate the efficacy and safety of antibiotics in non-[cystic fibrosis] bronchiectasis.”
For example, researchers in China are currently testing the immunostimulant OM-85 for non-cystic fibrosis bronchiectasis in children. Bayer is testing ciprofloxacin for bronchiectasis in a Phase III study. Ciprofloxacin is a powerful antibiotic that is already approved and used for several other types of bacterial infections. Other types of approved antibiotics are also used, but further rigorous study specifically in people with bronchiectasis is needed to confirm that they are effective and safe.
The study of treatments for bronchiectasis is clearly on the rise, which is important, since the sooner the condition is treated the less damage to the lungs can occur. Initial lung damage that leading to bronchiectasis frequently starts in childhood. Symptoms may occur later. Earlier and better treatments are important.

